Who we help
- GHANA
Case Studies:
Other Units We Support:
- SIERRA LEONE
Case Studies:
- Mendewa Hospital and Clinic
- Bo Children’s Hospital
- The Shepherd’s Hospice
- Holy Spirit Hospital, Makeni
- Bai Bureh Memorial Community Hospital
Other Units We Support:
- Kissi Town Community Health Centre
- TANZANIA
Case Studies:
- Kikavu Dispensary
- Chekereni Dispensary
- St Joseph’s Dispensary, Uchira
- Huruma Hospital
- Kilema Council Designated Hospital
- St Joseph’s Hospital, Soweto
- St Mary’s Dispensary KIA
- St Francis of Assisi School and Dispensary
- Kilema Hospital
- Kibosho Hospital
- St Camilius Health Centre, Mvimwa
- Kwediboma Health Centre
- Baraki Health Centre
- Bikira Maria Mama Wa Tumaini Health Centre, Masanga
- Rainbow Centre, Moshi
- Kibara Hospital
- Kitope Dispensary
- St Camillus Dispensary, Tomondo
- Bukwali Dispensary
- Makongoro Health Centre (AICT), Mwanza
- Sayusayu Dispensary
- Nyarambo Health Centre
Other Units We Support:
- Dr Atiman Hospital, Sumbawanga
- Kilolo Dispensary
- Kwamndolwa Health Centre
- Matai Health Centre
- Mgolole Health Centre & School, Orphanage
- Mvumi Hospital
- Mwayze Dispensary
- Namanyere Hospital
- Rosana Dispensary
- St Gemma's Health Centre, Lumuma
- St Martin de Porres Orphanage
- ZAMBIA
Case Studies:
Other Units We Support:
- MALAWI
Case Studies:
- Friends of Mulanje Orphans (FOMO) Orphanage, Mulanje
- Ndi Moyo Palliative Care Centre
- Madisi Mission Hospital
- St John of God Hospital, Mzuzu
- St Anne’s Hospital, Chilumba
- Nkhamenya Mission Hospital
- Nzama Health Centre
- Tsangano Health Centre
- Nsipe Health Centre
- St Martin’s Health Centre
- Namulenga Health Centre
- St Joseph’s Hospital, Limbe
- Pirimiti Community Hospital
- Matiya Health Centre
- Chiringa Health Centre
- Sukasanje Health Centre
- Fistula Care Centre
- St Peter’s Hospital, Likoma Island
Other Units We Support:
- Atupele Community Hospital
- Ekwendeni Hospital
- Kaseye Community Hospital
- Katete Community Hospital
- Mlambe Hospital
- Mzambhezi Hospital
- Neno Parish Health Centre
- St Patricks Health Centre, Rumphi
Does your health unit need our support?
CONTACT US NOWFriends of Mulanje Orphans (FOMO) Orphanage, Mulanje
FOMO is a community based orphan care programme supporting over 2,500 children through a network of 14 centres in Mulanje district of Malawi. It was established in 2000 and is a registered charity in both the UK & Malawi.
FOMO covers all aspects of the children’s welfare including formal and informal education, food security and production. The programme also covers pre-school, out of school activities and further learning through play schools, computer, driving and tailoring schools. It also covers the provision of school materials, personal items (Soap, clothes, blankets, and mosquito nets).
Healthcare is provided to the orphans as outreach from a central clinic. The clinic is staffed by a Clinical Officer, a Nurse and a Laboratory Technician. They can carry out minor procedures such as suturing and IV fluids and there is a laboratory for testing. Patients with medical conditions that cannot be treated by the staff at the clinic are taken to the local hospital. There are 9 beds for resting, but no in-patient facility.
Image below shows Inter Care medicines being unpacked at FOMO
Ndi Moyo Palliative Care Centre
To learn more about our partners at this health centre please visit:
Madisi Mission Hospital
Visit 2015
- Location: 80m KM north of Lilongwe. Dowa District. Lilongwe Archdiocese.
- Catchment population: 43,000
- Key staff met: Robert Jones and Oswald Yona Lungu (Administrator)
- Nearest referral unit: 80Km – Central Hospital Lilongwe
- Facilities: 123 beds in Maternity, Paediatric, male and female wards. Ambulance recently in an accident. 2 old vehicles and a motorbike. Lab, X-ray, Nutrition unit, HIV and TB programmes
- Staff: 6 clinical officers, 1 medical assistant, 25 nurses. Doctor visits regularly.
- Workload: 70 deliveries/month+ general outpatient and inpatient care
- Disease pattern: Standard for this area: Malaria, pneumonia, diarrhoea, sepsis, opportunistic infections associated with HIV, asthma, sexually transmitted infections +RTAs
- Estimated % of meds from IC: 5%
- Support from government and other sources: Vaccines, ARVs, TB drugs, Malaria tests and treatment from Central Government Stores. Staff salaries paid by CHAM
- Overview: Require another nebulizer. They would prefer to continue receiving 2 consignments from Inter Care per year but could collect parcels from the airport if necessary.
To learn more about our partners at this health centre please visit:
St John of God Hospital, Mzuzu
This hospital undertakes pioneering and extraordinary work in a country where there is hardly any provision for treating mental illness. The hospital is one of only three psychiatric units in Malawi which provide 39 inpatient beds and extensive specialist outpatient care. Furthermore, they deal with schizophrenia, depression, anxiety, drug-induced psychosis, epilepsy and clinics for the elderly. Although the environment is pleasant and rehabilitation programmes extensive, there are still significant problems with shortage of funds. it is difficult to get government funding for medicine and mental health care is expensive.
Moreover, there is a real difficulty sourcing psychiatric drugs. This is because their specialist nature means that they are not stocked by private pharmacies. More general medicines are used in the elderly clinics and for incidental infections and malaria in psychiatric patients.
Training in mental health is now a priority at St John of God, with over 150 nurses and 100 clinical officers now trained and degree courses available.
To learn more about our partners at this health centre please visit:
(pictures taken at visit in October 2012 and 2017)
St Anne’s Hospital, Chilumba
This small hospital with 54 beds is run by a clinical officer with surgical and obstetric emergencies referred to Karonga, an hour away along the main lakeshore road. Inter Care had direct experience of this when somehow we squashed into the ambulance with us a lady in obstructed labour, a guardian and a heap of luggage. (The outcome was good: amazing what a bumpy road can achieve it terms of progression in labour!)
When Sister Clementina arrived at Chilumba ten months ago she inherited a 10 million Kwacha (£10,000) deficit owed to drug companies. This is a common situation and means that hospitals buy from multiple pharmacies where they can extend their credit. The state of repair of buildings and level of equipment is poor, but this is hardly surprising. In particular, they asked if we could source a Doppler machine to assess better the need for maternity referral. The sisters’ accommodation is simple and power was a problem, but their welcome warm as ever.
To learn more about our partners at this health centre please visit:
(pictures sent via email in July 2019 showing the consignment we sent)
Nkhamenya Mission Hospital
Visit Report (October 2017)
This is 100 bed hospital with just ONE doctor. It is 60 Km on a good road from its referral hospital in Kasungu with a workload higher than expected from its catchment. This is because of patients crossing the Zambian border. There are approximately 77 deliveries per month and 65 outpatients per day. The hospital is situated on an entire mission complex which is beautifully kept and managed.
Requests were for surgical instruments which we could satisfy. They also requested for a biochemistry machine and cryotherapy unit. These items might, on occasion, be offered to Inter Care. It would also be a good candidate for an Aerogen Pro nebuliser.
Pictures taken in 2017 (Inter Care visit Nkhamenya and Ketete)
Nzama Health Centre
Our day at Nzama – 29th October 2019
Arrival
We spent 2 nights at Nzama HC, a very remote clinic along an extremely poor quality road. There is a new road being built but far from being ready so, along with poverty and unemployment transport is also a real problem. Sister Juliana is a sister of huge character and is a very a positive lady. All the sisters made us most welcome except for the cockerel who started crowing too early for sleeping!
The water and electricity is available and working perhaps 75% of the time. The medical assistant is Sister Theresa. Sister Juliana is wanting to recruit another medical assistant but before she can do so, she has to finish building a house for the new recruit – Thankfully it is almost ready!
At first glance
They have a new purpose-built Pharmacy, which was the best we saw on our entire trip. It has its own generator and air conditioning unit, a big relief from the heat of the outdoors!
We were informed that many of the patients must walk long distances, perhaps up to 4hrs and 50% of the patients are from Mozambique. They have a very old ambulance; however it can often be out of service being repaired for 3 months at a time making transferring patients a real issue.
The unit’s staff have very recently been trained by the government’s cervical screening program. The stipulation is that girls aged 15years and above are to be screened and every 3 years thereafter. Ladies who are HIV positive are to be screened annually. It is common for girls become sexually active from age 12 years old and so, by the time they are 18 years old they may be mother to 3 children.
Challenges
Malnutrition is a problem at Nzama. Here we met a single mum from Mozambique who had walked all the way, some 50-60kms, with her sick daughter who had malaria and who was also suffering from malnutrition. The little girl who was 1 year old was ‘in recovery’ from the malaria but still displaying severe symptoms of floppiness and malnutrition some 10 days on from arrival at the health centre. The young mother was very frightened and isolated as she had travelled alone on foot to reach the unit, but at some point, the Mother would have to start the long walk back home to Mozambique.
(Visit, October 2019)
Tsangano Health Centre
Our Journey
We travelled from Nzama HC south towards Mozambique for some 2 hours on very rough roads – This was not a journey for the faint hearted! We were hoping to meet the new Sister in Charge but unfortunately she was not there on the day so Patrick the Medical Assistant was our main contact here. Patrick was just finishing the morning out-patients clinic, which was conducted in a very small building that lacked an examination room.
At first glance
The area is very rural with poor sanitation so there are many diarrheal problems along with skin infections such as Scabies. When we visited, they had had rainfall a few weeks prior, so dysentery was a big concern because people were drinking dirty water. This is in a colder area of Malawi so chest infections such as pneumonia are more common however this also means that there is less malaria. The catchment area extends for 15-20kms meaning a 3-hour walk is often necessary for patients. The staff spoke of issues regarding knife crime in the vicinity. E.g. there is a local bar where the men folk drink heavily at weekends and fights often occur between the locals and those that travel from nearby Mozambique! Only the day before our visit a male patient who had been involved in a fight had had to be transferred to Ntcheu Hospital in their very old ambulance – a 3-4hrs journey, and can be a 5hr drive in the rainy season if the roads are passable.
Simply visiting Blantyre to buy medicines involves a journey of at least 5hrs each way so the staff only make the trip every 3 months or so. As for maternity services, the impact of this being a very rural clinic means that, for complications the journey to a hospital is too long and sadly, some babies/mothers do not survive. We were told that they lose 50% of their referrals in transit – a shocking statistic!
In terms of infrastructure the unit is working towards expanding their spaces. A new maternity unit has been built yet it is awaiting completion. The aim is that ultimately this development will provide more ward and clinic spaces, e.g. providing new-borns with their own ward area.
Summary
12 staff in total
- 8 nurses/midwives
- 1 Medical Assistant
- 1 Pharmacy Assistant
- 2 Accounts/admin staff
- Under 5s and maternal patients receive FOC medicines
- Charge all other patients
- However they make exemptions for some patients who cannot afford to pay – this is where donated medicines are used
Challenges
- Sanitation and hygiene in local area is very poor
- Trying to increase education in the villages
- Issue with fighting in the local areas at the bars. Large reason for this is that catchment area is on border with Mozambique, and there is lots of fighting between people from Malawi and Mozambique. Often use knives, which results in deep cuts and men admitted to Health Centre
- Only 1 Medical Assistant (no Doctors or Clinical Officers) – usually seeing over 50 patients a day
- Ambulance to transfer patients to other hospitals is too old and needs to be replaced. The ambulance struggles with lots of non-tarmac roads in the area
- Lots of cases of diarrhoea resulting from rainfall a couple of weeks ago and subsequently people drinking from wells
- Not enough rooms and beds to treat all patients, resulting in overcrowding and patients in corridors
- Children with diarrhoea are in same room as newborns and any other diseases children are being treated for
- Not enough staff houses – 3 houses for 12 staff
- No NRU for nutrition – Patients get transferred from here to Nzama who have nutrition unit
- No generator currently, for when they lose electricity
- Used to have lots of neo-natal deaths – they often need to transfer mothers to Ntcheu
- Now 50:50 chance of survival
- Patients are usually referred to Ntcheu which is 80km away and takes 3-4 hours by ambulance. In critical cases this has led to patient deaths or unnecessary added complications
- Contributes to number of neo-natal deaths
Medicines most needed
- Ferrous Sulphate – prescribed to pregnant women
- Prednisolone
- Amoxicillin
- Cloxacillin
- Ciprofloxacin
- Paracetamol and Ibuprofen
- Co-Trimoxazole
- Hydrocortisone
- Benzyl Benzoate – for treating scabies and skin conditions
Commonly treat for
- Lots of skin conditions and eye conditions
- Scabies due to lack of hygiene in local villages – lots of children in particular
- Lots of patients treated for severe diarrhoea due to poor sanitation and hygiene in local villages – treated with ORS, Zinc and Loparamide
- Lots of conjunctivitis, especially among young children
- Not many cases of malaria here, as higher up and has cooler temperatures
- Pneumonia and diarrhoea have highest number of patients treated for
- Some dysentery and Gastro-enteritis also
Other observations
- They buy medicines from Blantyre quarterly using old ambulance.
- Patrick (Med Asst) has seen more than 50 patients by 11am today.
- Catchment area is large about 15km (25,000 people). Patients often walk over 3 hours to get here
- Children with diarrhoea are in same room as newborns and any other diseases children are being treated for
Female ward
- Patients bring their own linen sometimes as the Health Centre does not have enough for all patients
- Very cramped. Some patients are sharing beds
- There are mothers with new babies, mixed with a range of other illnesses. For example there is currently a patient being treated for dysentery
- We observed that although the Health Centre is undoubtedly cramped, it could be organised better. For example they have an entire room allocated for relatives next door, which we perceived would have been better used to expand space for female patients
Male ward
- No patients in male ward currently
- 7 beds
- Larger ward than Female ward that only has 3 beds. Could they switch male and female wards to better utilise space
- With the Health Centre being so understaffed, and the burden placed on existing staff these are considerations, which perhaps the staff do not have time to make.
(Visit, October 2019)
Nsipe Health Centre
Nspie is a small village located around 16km east of Ntcheu and about 140km north of Blantyre and 180km south of Lilongwe. The clinic serves 36 villages in the surrounding area, with an estimated population of 25,331. The clinic provides outreach services to the villages, reached by bicycle. The clinic also serves people from the wider area as the government facility in the neighbouring area has no maternity care.
The electricity supply and water supply are not perfect but are manageable. This unit also has a good working relationship with the government and a local hospital at Ntcheu and, works alongside 36 outreach clinics. The unit has access to shared vehicles/bikes, and also medicines if needed.
The main issue here is the infrastructure – the lack of buildings and beds! E.g. the labour ward has only 2 beds so, at busy times some babies are delivered in the corridor.
Mothers and babies usually only stay for 24hrs, not the usual 48hrs, due the lack of beds.
The electricity typically goes off for 3 hours at a time, once or twice a day. The water is served by an electric pump, so this also causes a problem. They do have a backup generator which they use when necessary. Communication here is challenging, they have to travel to Ntcheu to access the internet. Medicines are collected by ambulance from the post office in Ntcheu, and Ntcheu District Hospital is the closest hospital for referrals. The clinic uses a WhatsApp group where they can discuss cases with staff from the hospital to receive guidance before making a referral.
The clinic is run by the Sister in Charge, Sister Josephine, who is a trained nurse midwife. The clinic has an SLA with the government for maternity and care of children under 5. They also provide HIV, TB, malaria, nutrition and vaccinations. All of this is provided for free. If patients come for other conditions, they pay 500 Kwacha (50 pence) for a consultation and the same again if they need a bed for the night. Medicines are charged for on top unless they have donated medicines available. The clinic has not been paid by the government for over six months.
The clinic purchases most of its medicines 4 times a year from wholesalers in Blantyre who let them take items on credit.
Inter Care is the only source of donated medicines, which make up about 5-6% of their stock.
The pharmacy is managed by a nurse midwife, with support from the medical assistant. If they run out of a medicine, they try to trade with the government hospital. The pharmacy keeps purchased and donated medicines separate. There is no temperature management in the pharmacy, they are just kept in a dark room.
Each month, they see around 4,080 outpatients and 240 inpatients. There are 56 beds. On average they deliver around 70-80 babies a month, but last month it was 110 deliveries. There is no incubator so premature babies receive Kangaroo care.
Most common health issue seen include skin conditions, upper respiratory tract infections, pneumonia, gastrointestinal illnesses, diarrhoeal disease, sepsis, malnutrition, malaria, eye conditions, STIs including HIV, trauma or heart conditions. There is currently an outbreak of scabies in the community.
(Visit, October 2019)
St Martin’s Health Centre
At first glance, we notice that the unit is very poor with little in the way of facilities. The outreach clinics are remote and difficult to get to with a very old ambulance which is not even a 4×4 wheel drive. Both electricity and water are major issues for the clinic and there is no money available for either. To make matters worse the water pump at the unit is currently broken.
Wellington the Medical Assistant is good however he has to see 80+ patients per day! -A huge workload. See his full story here
They have an under 5’s clinic most days however, it is held in a building resembling a cow shed which does not have seating for those waiting to be seen. Their laboratory is of an extremely poor standard, as is the pharmacy – which provides very little education for the staff.
See Zione and Mara’s story here
The unit is very reliant on the banana plants however, after devastating floods in 2015 a crop failure followed. The government has ordered the locals to uproot diseased plants but they are refusing and consequently are still having considerable crop issues. Bananas are a main staple food of the area i.e. we had bananas every day at least twice in all different forms hot and cold, so it was clear to us that a crop failure has a direct and huge impact for the local people.
Challenges
- Only Ambulance keeps breaking down
- Road has only been tarmacked in last 3-4 years. Up until this point they faced a lot of issues in terms of transport, access and remoteness.
- They have a well and a pump. However they have had difficulties accessing, so sometimes have to bring water back from a bore hole some distance away.
- They would like to introduce a solar pump
- Sometimes go days without electricity and don’t have a backup generator.
- Only 1 Medical Assistant (no Doctors or Clinical Officers)
Medicines most needed
- Amoxicillin
- Ciprofloxacin
- Co-Trimoxazole
- Paracetamol
- Ibuprofen
- Also mentioned Salbutamol tabs are in low supply and would be most needed donated
- Metformin (Glucophage) also needed for diabetic patients
- They received a delivery from Inter Care 6 weeks ago
- Ciprofloxacin and Amoxicillin tablets they received have been used already
- No taxes on receiving stock from Inter Care
Commonly treat for
- Malaria
- Pneumonia
- Skin Conditions
- Epilepsy
Other observations
- Nearest referral hospital is Malamulo Hospital 13km away.
- If suspected Sepsis or Meningitis they refer to nearest district hospital
- A lot of patients die in local villages and are brought to HC to confirm death
- There are posters up with preparations for Ebola in HC and external programme across district.
- Some people are affected by Cyclone Idai in lower parts of catchment area
- Houses collapsed and some children died
- Some families houses have been rebuilt and have moved back
- Banana crop failure in area
- They purchase medicines from Blantyre once a month
- However have real difficulties with transport and fluctuation of prices
- Purchase from Unichem, Worldwide and Pharmavisit (?)
- Stock outs not always common, but they have a lot currently as coming up to busy period before rainy season
- When Cipro runs out, they use alternative medicines, not always as effective
(Visit, October 2019)
Namulenga Health Centre
Namulenga is located about 45km away from Blantyre. It was built in 1968.
It is a small Health Centre with only a Medical Assistant prescribing medicines, along with 5 nurses/midwives, 1 lab attendant and 1 pharmacy assistant for a catchment population of just over 11,000.
There is no Clinical Officer or doctor on site, they are only visited by a doctor from the regional hospital once every three months. These visits provide an opportunity to discuss complicated cases, and raise wider issues affecting the clinic.
- The clinic contains a 10 bed maternity ward, and a 10 person general ward.
- The health centre provides antenatal care and deliver 10-20 babies a month
- The clinic provides maternity services, and services for patients with HIV and TB.
They had installed solar panels recently but only to power the refrigerator so even the pharmacy was very hot. On average the electricity is off for 8 hours a day. They have a water pipe from the mountain area but often it delivers a very low pressure so, they must use the borehole at the primary school.
They have a very old ambulance however, when we visited it was in for a service so, they had no means of transport other than bicycles.
The equipment on the wards and the labour unit was in a good condition but the laboratory was very poor!
They were in desperate need of some microscopy charts for the wall.
Staff accommodation was minimal with only 3 beds for the 5 staff meaning that 2 staff members are required to sleep outside every night!
SISTER MARTHA’S STORY (Medical Assistant)
“This morning I treated a boy of 12 years old. His mother was away, and he had tried cooking Nsima [cooked, ground white maize flour – a staple food] for himself, and was burned by the flame. I was able to give him painkillers and dressings, but we have run out of silver sulfadiazine cream, so I had to send him to the hospital. That is unfortunate because we would like to be able to treat that kind of simple condition here, without making him make a long and unnecessary journey to the hospital. “
“One of the items we recently received from IHP through Inter Care, were some children’s ear thermometers. They are brilliant! They are fast, they are accurate, and they are good for babies who wriggle!”
See Sr Martha’s full story – Download here
St Joseph’s Hospital, Limbe
We spent the day at the hospital which is situated a 45-minute drive from Lunzu where we were staying. The Director Sister Mercy is a busy lady, and we spoke at length to Michael, Head of the Medical Team. The hospital has a very busy OPD (outpatient department) seeing on average 80-100 patients per day. The hospital has 198 beds – on average 50-60 are occupied overnight.
We visited the laboratory which is small by our standards. They have a small chemical analyzer (see image) which had been funded by an external company, however the funding had stopped so the machine was no longer in use. Furthermore, they were lacking an incubator so were unable to process any cultures – this was a big challenge for them. They were however using the Gene Xpert program to support TB screening and, a new development is that they are now starting cervical screening programs.
The pharmacy department recently moved into a new building and was well organized however, sourcing products remains an issue due to ‘out of stocks’ and having to buy from private pharmacies. One of the major challenges faced by the hospital was security and loaning equipment to patients, e.g. crutches which were subsequently not returned.
In the afternoon, we visited the Training College, which has always offered Nursing and Midwifery training. However, in 2017 they started offering Pharmacy Assistant training as well. The capacity of the college is 480 students, there are 84 employees of whom 28 are academic staff. Nursing Midwifery Diploma is a 3-year course and the Pharmacy Assistant Certificate 2 years. They had recently purchased 70 BNFs at a cost of £350.
We suggest this would be a good place to provide teaching aids/appropriate books to in the future.
Sister Mercy has excellent contacts with all the health units in the area and would be willing to work with Inter Care to facilitate distribution of goods across the area when we can send a container.
(Visit, October 2019)
Pirimiti Community Hospital
Pirimiti Community Hospital has benefitted from recent building improvements. The new building is exceptionally clean, well-organised and is unrecognisable from when Inter Care had visited previously in 2009. Sister Mary Njuguna (from Kenya) is the Hospital Director.
Medical Provision
The patients that attend the hospital are cared for in the main maternity wing, along with the surgical cases. They have no anaesthetic machine and use spinal anaesthesia for C-sections. They have 350 deliveries per month, of which approximately 65 are C-sections. This number is relatively high because complicated cases are referred to them from five surrounding health centres – two are NGO’s (including Matiya Health Centre) and three are government units.
The other wards are male, female and paediatric – seeing many cases of malaria, urinary tract infections, skin conditions and pneumonia. Road traffic accidents tend to be referred to Zomba General Hospital.
Medical Conditions
Malaria is the most common ailment treated, followed by urinary tract infections, pneumonia, skin conditions, and sexually transmitted diseases.
A young man being treated at Pirimiti
They are very busy
In addition to the number of births (350), they treat over 50 inpatients, and 1,200 outpatients each month. They also see over 3,500 patients each month at their various clinics.
Inter Care’s Impact
Inter Care has supported Pirimiti Community Hospital with the provision of medicines and health care goods for 16 years. In September 2021 Inter Care funded £8,888 worth of vital medicines and health care goods delivered through medical distributor / supplier Action Medeor, our partner in Malawi.
Matiya Health Centre
Matiya Health Centre is on the main road to Zomba which is tarmacked until the last 7km where the surface changes to marram roads. It is a small health centre with 28 beds and a high volume of patients. It is extremely busy serving a large catchment population of 48,278.
It has a very poor infrastructure. Only 4 of the 11 staff can be housed and the rest sleep outside in tents, yet they do amazing work.
The buildings were damaged by Cyclone Idai which hit the country in 2019. Sadly, many of the population lost their lives during the cyclone and many have been left homeless by the destruction it left behind.
Medical Provision
A small unit with 28 beds, Matiya treats over 130 inpatients and 1,800 outpatients per month. The unit also supports a mammoth 96 villages per month with outreach services. The average number of deliveries each month is 126 babies. The most common conditions they encounter are respiratory tract infections, followed by hypertension, sexually transmitted diseases and skin conditions.
Medical Staff
With 1 Clinical Officer, 2 Medical Assistants and 12 nurse/midwives, they manage to provide a considerable outreach service.
Inter Care’s Impact
Case Study: Kenneth Golosi, Matiya’s Clinical Officer recounted details of a patient he had seen that morning – a 2-year-old child who was HIV positive. His mother had carried him 8kms on foot, wearing no shoes, after the boy had suffered for three days with a fever and a cough.
On examination his temperature was 38oC and he was irate, pink/febrile and clearly distressed. Kenneth carried out a physical examination which showed mild cramps, however the abdomen was clear. The treatment plan was to test for malaria first which proved positive. He also suspected an acute respiratory infection. The initial treatment given was antibiotics (amoxicillin) for seven days coupled with paracetamol for three days for pain relief. All the treatments given were donated by Inter Care.
Sr. Stivelio Macloud – Sr. in Charge
Also donated was a crocheted blanket for baby Innocent who had been born with six digits on each hand (knitted by a local Inter Care supporter group based in East Goscote, Leicestershire).
A recent quote from Sister Stivelio “The supplies we receive from Inter Care are 100% suitable for our needs.” underlines not only the importance of Inter Care’s support to Matiya, but it also emphasises the value of the Inter Care’s policy of, ensuring that we only supply what they tell us they most need.
Chiringa Health Centre
One of the smallest, and most remote units partnered by Inter Care, Chiringa has only 25 beds supporting a local population of 1,700. Being near the Mozambique border they receive many patients from across the border. When Inter Care visited Chiringa in 2019 we met with Sr. Rhoda Bendala who showed us around a very clean and organised facility. They told us that their water pump had recently been stolen, so they were having to rely on a bore hole.
Staffing
They have no doctor but do have a clinical officer, eight nurses/midwives and a medical assistant. They average 30 deliveries a month, and the conditions they most often treat are: malaria, pneumonia and hypertension.
Sister Rhoda Bendala at Chiringa Health Centre
Inter Care Impact
Inter Care has supported Chiringa Health Centre with the provision of medicines and health care goods for 10 years. In September 2021 Inter Care funded over £3,000 worth of essential medicines delivered through medical distributor / supplier Action Medeor, our partner in Malawi.
Sukasanje Health Centre
Sukasanje, with 45 beds, is a 70-minute drive from Blantyre on a good road to the Mozambique border, then 70 minutes on a marram road which requires a 4×4 vehicle and is impassable in the rainy season. The unit is situated at the foot of Mulanje Mountain and as such has good access to piped water from the mountain. Visitors are extremely rare and very little English is spoken.
They have no IT equipment or internet connection, so the only method of communicating is via WhatsApp or by postal letter.
Staffing
Due to its remoteness staff turnover is high and they struggle to recruit and retain medical staff. They have one very young medical assistant and nine nurse/midwives.
Medical Provision
The local population of 25,000 are mainly unemployed and many patients come across the border from Mozambique (it is literally on the border) to receive medical treatment. On average they treat over 1,500 outpatients and deliver 80 babies each month. The main conditions they are faced with are:
- Malaria
- Pneumonia
- Asthma
- Respiratory Infections
- Hypertension
Needs
They keep very few patients in overnight but when they do, they charge the equivalent of 50p per night. Staff made requests to Inter Care for mattresses because those that they have are in a terrible condition with the foam being visible. Also, all bedsheets were missing – consequently patients had to use their own chitenjes (large pieces of coloured fabric) as the health unit could not provide any linen.
Inter Care Impact
When we visited in 2019, they asked if we could supply bedlinen and mattresses; this is not the usual request that we respond to as it is not directly medicines or Health Care Goods, however the One Wish Project could enable us to supply these if still needed.
Inter Care has supported Sukasanje Health Centre with the provision of medicines and health care goods for 16 years. In September 2021 Inter Care funded over £16,000 worth of vital supplies, delivered through medical distributor / supplier Action Medeor, our partner in Malawi.
Fistula Care Centre
Visit report
The Centre runs a training programme for surgeons, nurses, medical and clinical officers. These are all trained by a Malawian fistula surgeon.
This centre is located in the grounds of Bwaila Hospital, Lilongwe and has 35 beds and an operating theatre.
The unit in Lilongwe sees and treats up to 300 women per year with vesico-vaginal fistula, (VVF), partly as ongoing work and partly at twice yearly ‘camps’. These run for an intensive 10-day period, during which 90 women are treated. These camps also take place in other Fistula Centres in Zomba and Blantyre. The overall success of surgery is 91%.
Overview/Case Study
Obstetric fistula is a devastating childbirth injury caused by prolonged obstructed labour. To elaborate, it causes incontinence and infection and social stigmatisation. Between 50,000 and 100,000 women each year are affected each year globally. The Fistula Care Centre is a national specialist organisation treating women with VVF, usually caused by the ‘3 delays’ in maternity management.
The Centre takes a holistic approach to the care and rehabilitation of patients. They draw on rehabilitation, education and an empowerment programme. This includes access to micro-finance, a solar project where the women are given and taught to use a portable solar panel unit and literacy and numeracy classes, as well as lessons in arts and crafts.
The Centre has also established an Ambassador Programme where patients return to their communities and talk about the condition and its effect on women as well as supporting other women with VVF to seek support at the Centre. Despite being relatively well funded, the Centre still cannot access all the medicines and medical supplies it needs as there is a shortage of availability from the government.
They are therefore continually in need of antibiotics, painkillers, plasters and catheters. They were also very keen to receive Afripads (reusable sanitary pads) to add to the “welcome box” the women receive on arrival at the Centre. The approach taken to supporting the women was very impressive. .
To learn more about our partners at this health centre please visit:
St John of God Hospital’s Official Site
(pictures taken at visit in 2015)
St Peter’s Hospital, Likoma Island
St Peter’s is a 52-bed Anglican hospital. It is beautifully situated next to the historic cathedral on Likoma Island in the centre of Lake Malawi. It is a busy place run by 2 clinical officers, 1 medical assistant, 12 qualified nurses and 1 laboratory technician caring for 4,450 Outpatients and 120 Inpatients per month.
Upon our visit in October 2017 we found it to be rather isolated i.e. the nearest referral centre 70km away by an infrequent and somewhat unreliable boat service. To exacerbate things the hospital boat was broken so emergency referral and the transportation of medicines is particularly problematic. We also noted a significant influx of patients travelling to St Peter’s from the nearby Mozambique coast which, effectively doubled the expected number of patients. Staff told us that the isolation issue also means that it is very challenging for them to recruit and retain staff.
Despite the absence of a qualified doctor the hospital needs to be able to cope with most eventualities including surgery and encouragingly, we learned that one of the clinical officers is currently studying for a degree in mental health. Their stocks of medication are supposedly supplied by the government through central medical stores but we are told that time after time this proves unreliable. Furthermore, it does not begin to keep pace with an extra influx of patients, leading inevitably to frequent shortages.
From our tour, we found Hospital Administrator Francis Vuma to be outstanding in his service to the hospital and, going forward we anticipate his advising Inter Care with local knowledge to improve the bespoke medical aid we can provide to Malawi in general. For St Peter’s Hospital Mr Vuma said “Funding for medicines and medical supplies, equipment are a challenge” Inter Care currently send consignments bi-annually which include medicines and medical supplies.
Mendewa Hospital and Clinic
Founded only in 2018, Mendewa is a small hospital, 8 miles from the town of Bo, with a catchment population of 5,000. The community in their area is impoverished, with no access to electricity, running water or main roads. Rates of illiteracy and under age pregnancy are high, poverty and poor health are debilitating factors in the area.
The Hospital: With 15 beds, they treat 225 adults and 720 patients under 18 each month. The opening of the hospital has helped to improve the overall health and wellbeing of the community, and since it has opened it has helped to reduce the infant mortality rate as well as the rate of deaths related to malaria and typhoid.
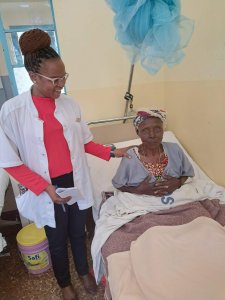
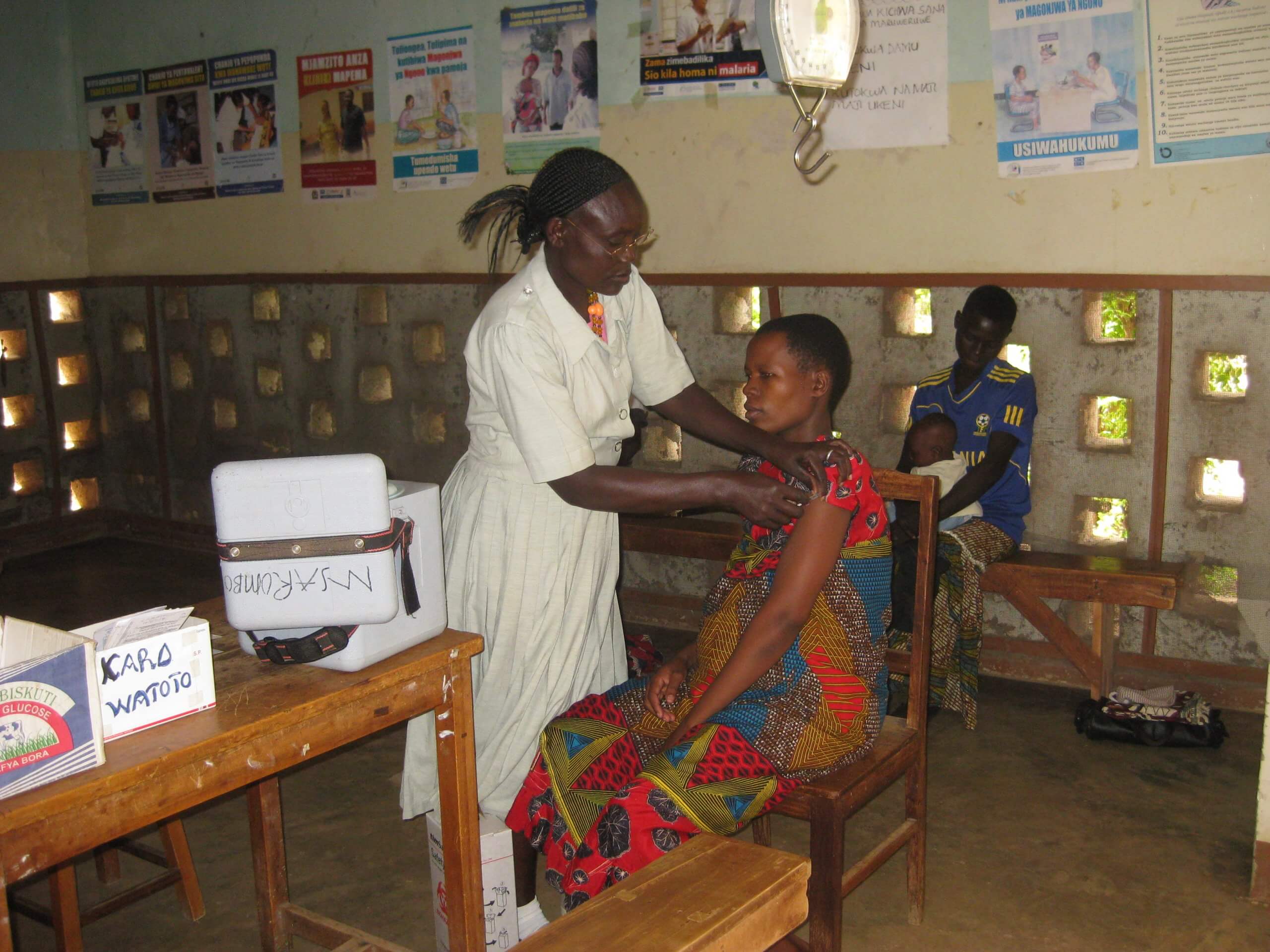
 Immunisations for Pregnant Mothers
Immunisations for Pregnant Mothers
Medical Priorities: Malaria and typhoid are their biggest medical problems, both in terms of cases presenting and as a cause of death.
 Measles/Rubella Outreach Programme
Measles/Rubella Outreach Programme
Medical Staff: There are 6 nurses and a midwife, a doctor visits once each week.
Inter Care’s Impact: As well as the direct medical aid, we also supply medical books wherever we can and where there is most need. Mendewa was one such beneficiary: “The Medical books have proved a big hit with our qualified staff and our student nurses, we are now hoping to gather enough to start a small library in the future, as books of this nature are rare and expensive in Sierra Leone. The Nurses have asked me to give you all a big Thank You!”
 Student Nurses with their new text books supplied by Inter Care
Student Nurses with their new text books supplied by Inter Care
Inter Care’s Impact: Mendewa Hospital is a recent addition to the health units supported by Inter Care, their first shipment of medical aid was delivered in May 2021. Within 6 months well over 100 patients had benefitted from this aid.
Bo Children’s Hospital
Sierra Leone is a country which has a very high infant mortality and very low life expectancy, largely down to the lack of availability of treatment. According to the World Health Organisation the likelihood of dying before the age of 15 is more than 50% for both males and females.
The Bo Children’s Hospital is only the second children’s hospital to open in the history of Sierra Leone. Since its inception in June 2012 it has successfully treated over 30,000 children and is making a tangible difference in the community, especially for the helpless young children who are in desperate need of medical care. The biggest impact the hospital has made since it opened its doors has been saving lives from preventable conditions such as Malaria, malnutrition and diarrhoea.
Childrens’ Outpatient Clinic
Medical Staff: they have 17 nurses, 3 clinical officers and a doctor who visits once a week. The staff are all from the local community and take full responsibility for running the hospital.
 Inter Care volunteer Imelda visiting Dr Sesay in August 2021
Inter Care volunteer Imelda visiting Dr Sesay in August 2021
Medical Conditions: Malaria accounts for about 48% of out-patient attendances, it also accounts for about 25% mortality in children under five, another 25% of which die due to malnutrition. Other than Malaria the main conditions seen are Diarrhoea, Tuberculosis, HIV/AIDS and Pneumonia.
Medical Facilities: This much needed hospital has 25 beds for both day and overnight admissions whilst also providing outpatients clinics, imaging and laboratory facilities, a pharmacy and minor surgery. A Triage and Isolation Ward have been added to the original building to handle the outbreak of infectious diseases. It also supports the parents by providing education about disease prevention and hygiene issues.
 One of the wards at Bo Childrens’ Hospital
One of the wards at Bo Childrens’ Hospital
Covid 19: the pandemic has had a severe impact on the hospital as it was used as a holding and treatment centre for Covid 19 patients. This not only reduced significantly the services they provided, but has also caused patients to be reluctant to attend due to the stigma of Covid.
The Shepherd’s Hospice
“The Shepherd’s Hospice Sierra Leone believes that all people deserve compassion, honesty and comfort as they deal with a life-threatening illness”
The Shepherd’s Hospice is unique in Sierra Leone as it is an organisation specialising in palliative care for the terminally ill which they also provide training for. The hospice does not operate in the same way as a traditional hospice in the UK in that it mainly provides support to families who take home terminally ill patients and helps them provide palliative care at home.
 Background: The Hospice was established as a local, non-governmental organization in 1994 with a mission to promote palliative care and health development in the Western Area of Sierra Leone. They moved to a purpose-built facility with inpatient, outpatient and home-based care in a more peaceful, rural site, in Waterloo on the outskirts of Freetown, in 2016. The population of their catchment area is over 250,000.
Background: The Hospice was established as a local, non-governmental organization in 1994 with a mission to promote palliative care and health development in the Western Area of Sierra Leone. They moved to a purpose-built facility with inpatient, outpatient and home-based care in a more peaceful, rural site, in Waterloo on the outskirts of Freetown, in 2016. The population of their catchment area is over 250,000.
Medical Staff: They employ 1 full time and 1 visiting doctor, 2 Community Health Officers, 16 nurses & a community health nurse. They visit patients in their homes and monitor their care, as well as making sure they have the medicines etc. that they require. Recently many staff from international medical teams have returned to their own countries due to Covid 19, leaving the hospice short-staffed.
Homecare: They provide Medical Consulting and Nursing Care at home as well as Phone Support for people who have serious illness but are too weak to travel, or who are unable to enrol in inpatient hospice.
 Inpatient Hospice: (24-hour symptom management); suitable for patients suffering severe symptoms which require intensive palliative care e.g. pain, difficulty breathing, nausea, and end-of-life symptoms which their families cannot manage at home. On average they have 27 inpatients per month.
Inpatient Hospice: (24-hour symptom management); suitable for patients suffering severe symptoms which require intensive palliative care e.g. pain, difficulty breathing, nausea, and end-of-life symptoms which their families cannot manage at home. On average they have 27 inpatients per month.
Medical Conditions: They focus on chronic diseases such as HIV/AIDS, TB and cancer. They mainly treat symptomatically for pain but also treat opportunistic infections. In addition to these they also run regular clinics for Diabetes and Hypertension.
Outpatient Clinic: The hospice provides primary care for the local community seeing over 100 patients per month for review of their medical problems or nursing needs e.g. wound care.
Other activities: They run a national TB program that involves a network of training officers going out into the provinces on motorcycles. This involves providing training and medications as well as setting up sputum labs where none are currently available.
Inter Care’s Impact: We recently received a heart-warming note from Gabriel Madiye, Executive Director of The Shepherd’s Hospice. He wrote “we bring some patients to the hospice centre for out-patient care, where patients are able to travel or assisted by the hospice vehicle. We are grateful that your donations are helping us reach the unreached, poor and vulnerable patients like Mama. She is a 27 year single unemployed mother living in Jui village and has suffered rejection and stigma because of her gangrene but is now being treated. Your generosity touches people in our deprived communities.”
Holy Spirit Hospital, Makeni
Founded in 2002, Holy Spirit Hospital is located in Masuba, 55km South of the city of Makeni – the largest city in the Northern Province of Sierra Leone. The dedicated staff in the hospital serve a catchment population of 600,000.
 Dr Turay, Medical Director of Holy Spirit Hospital visits the Inter Care warehouse
Dr Turay, Medical Director of Holy Spirit Hospital visits the Inter Care warehouse
Hospital Facilities: this is a 75 bed hospital with wards serving a varied range of needs e.g. medical, surgical, paediatrics, and general. Other key features include 3 Operating Theatres, a Laboratory, a Pharmacy, and a new, recently opened, Maternity Wing.
They also have 3 ambulances and a van to help with transportation of their staff e.g. for home visits.
Medical Resources: The hospital is looked after by a total of 40 staff. These include; 3 resident doctors, plus 1 visiting part time, 16 nurses, 4 midwives and 3 laboratory technicians.
They are very busy: They treat over 11,000 patients each year. 2,000 of these patients are in their teens and 4,000 are children under 12 years old. Each month they treat approximately 9,500 Outpatients and look after 90 Inpatients. In the maternity wards, between 5-7 babies are born every month and take their first breaths at Holy Spirit Hospital.
Medical Conditions: Malaria, hypertension and gastritis are the most common conditions encountered at the hospital.
Outreach: They have outreach programmes to 4 local villages covering, General Medical, Under 5s and Maternity.
The challenges: The Ebola epidemic of 2014-6 had an enormous impact on the hospital, and it is still recovering. The economic situation remains extremely challenging, aggravated by the high incidence of Malaria, Hepatitis B and HIV/AIDS. They have difficulties with the availability of required medicines. Furthermore, there are challenges with counterfeit medicines entering their supply chain.
 Holy Spirit staff sorting dressings sent by Inter Care
Holy Spirit staff sorting dressings sent by Inter Care
Quote from Dr Patrick Turay, September 2021: “they have been able to carry out reconstructive surgery due to the quality and effectiveness of the supply of dressings”
The Holy Spirit Hospital’s role with Inter Care Containers
Dispatching a container packed with medical aid to a country brings great advantages, but also logistical problems. The advantages are that large, heavy items, far too expensive to send by air, can be sent economically by Inter Care. One of the disadvantages is that all that aid arrives at the same place, and that the hospitals, health units and dispensaries for whom the aid is intended can be dispersed far and wide.
Inter Care supports 7 such scattered units in Sierra Leone, and we are extremely grateful that Dr Turay at Holy Spirit Hospital agrees to take delivery of the container, and to arrange the distribution of its contents amongst all the country’s recipients.
Unloading the container at Holy Spirit Hospital
“We assure you that these supplies will be used well for the good of the patients. You are a true partner.”
Reaction from Dr Turay on arrival of the first container
Bai Bureh Memorial Community Hospital
Founded in 1971 as a private hospital Bai Bureh and is located in Lunghi, across the water from Freetown. Bai Bureh is only accessible via very poor quality roads. Today, this 50 bed hospital provides healthcare cover to a relatively large 800,000 catchment that includes the airport and its workers, as well as some people who come from nearby Freetown.
Medical Provision: With a total 41 staff including 4 doctors, 1 pharmacist, 25 nurses and 2 midwives hospital treats around 209 Outpatients and 184 Inpatient admissions each month.
Inter Care’s Impact: Inter Care started supporting Bai Bureh Hospital after visiting in February 2010. We knew we could provide basic medicines and dressings. Over 4,700 patients each year benefit from the free medicines provided by Inter Care.
Inter Care Visit to Bai Bureh September 2022: An Inter Care volunteer visited Bai Bureh to meet the staff, inspect the facilities and enquire about their current problems. It is extremely important to visit the medical units so that we can ensure that the support provided by Inter Care is appropriate (i.e. what we send is what they need), and also that it is used appropriately.
Particular problems identified this time included:
- Shortage of drugs: actually getting hold of the medicines they need, but also obtaining drugs locally of the highest quality (see the Case Study below)
- Electricity supply: the supply is unreliable and unpredictable, they have had spells of 3 months without any electricity so have to rely on a generator and solar unit
- Shortage of laboratory testing equipment
- Lack of equipment for the operating theatre (e.g. monitors, Autoclaves)
- Transport: in the rainy season the condition of the roads is so bad (potholes and flooding) that getting to work is a problem for the staff, they are often delayed as the only means of transport they have is bicycle. It is also, clearly, a problem for patients.
Mariana’s Story
Mariana is 71 years old woman who had travelled all over the country for ten years in search of proper treatment for her illness, but she could not find anywhere that could heal or stabilise it.
When she first visited Bai Bureh Hospital in 2019, she was diagnosed with Severe Malaria and Diabetes and was admitted immediately, and her treatment commenced straight away.
A few days later the malaria was gone and there was some massive improvement in her general health condition. Her daughter, who had been travelling with her right round the country, visited her and was so happy (and surprised) at the improvements that had taken place.
She decided to see Doctor to thank her and to ask what sort of treatment was administered that had made so much improvement in her mother’s life. The Doctor explained that it was the quality of drugs that were administered to her. Bai Bureh Hospital had just received their supplies from Inter Care which included Metformin and Glibenclamide which were given to Mariana.
Before coming to Bai Bureh, Mariana had been seen and treated by many health professionals, but she was not seeing any improvements because of the poor quality of the drugs she had been given. Sierra Leone is full of many counterfeit drugs and this is deterring the work of many health professionals in the country.
Mariana and a lot of poor women and men in the community have been placed on regular visits to the hospital to monitor them continuously as they respond to medical treatment. They are always thankful to us and the entire team at Inter Care for giving them such expensive and good quality drugs free of charge.
Bai Bureh’s Clinical Officer, Daniel Hassan Larkoh, explains why Inter Care is so important
On behalf of Bai Bureh Memorial Community Hospital I will like to register my sincere thanks and appreciation to the entire Inter Care family for the huge support over the years.
Because of you our facility has been able to maintain its quality service delivery over the years and even in difficult times. At a time when a lot of facilities cannot function properly we were here delivering quality medical services to our patients.
The quality of the drugs we receive from you cannot be compared to this country because most of the drugs a lot of clinics and hospitals are dealing with in Sierra Leone today are counterfeit drugs from Asia and other African countries. To be honest with you Inter Care is setting us apart from the others in medical service delivery in this part of the country and beyond.
Kikavu Dispensary
Kikavu Dispensary serves a large, very poor population which is swelled by workers from the nearby sugar cane plantation. The Dispensary is relatively well resourced and run to a high standard by Dr August Temu and his team. It is supported by Health Amplifier UK, which amongst other things, funds the staff salaries. An Inter Care volunteer doctor, Julian Brown, was instrumental in setting up this charity following a visit to Kikavu in 2014.
Julian Brown during the expansion of Kikavu Dispensary
An innovative Community Care Plan is run at the Dispensary by Dr Temu and several community volunteers. They work with people to educate on basic health, nutrition and disease prevention. Any household which, with the support and monitoring of the volunteers, actions 10 required steps are awarded a Patient Passport at the dispensary and receive free health care and lab testing. The 10 steps include having a toilet with handwashing facilities, a rubbish pit, a mosquito net over every bed, under 5s being inoculated, growing 2 fruit trees (provided by the clinic), and only drinking boiled water. There has been a significant improvement in health in the community as a result of the Care Plan.
Lydia received her Patient Passport in 2022 – this is her home
Medical Provision: The most common conditions which are treated at Kikavu Dispensary are upper respiratory infections, urinary tract infections, gastro-intestinal diseases, skin diseases, hypertension and diabetes type II. A mother and child centre has also been opened in recent years and the first baby was born there in 2022.
One of the major problems which Kikavu faces is staff retention. They cannot match the salaries offered at government facilities and so there is the constant risk that staff, and in particular the Clinical Officer, will leave.
Inter Care’s Impact : Inter Care has been working in partnership with Kikavu Dispensary since 2016, providing vital healthcare goods and medicines.
The new mother and child clinic
Chekereni Dispensary
Chekereni Dispensary is in a remote location 15 kms outside of Moshi – it serves a rural, poverty stricken population who are largely unemployed. The dispensary has many serious issues, including leaking roofs, an inadequate water supply, an insecure, unfenced site and a serious lack of medical equipment and medicines. The unit doesn’t have a back-up generator, so when the electricity fails, the staff are forced to use the lights on their mobile phones.
 Fr Priscus stands underneath the leaking roof which is causing damp in the maternal unit
Fr Priscus stands underneath the leaking roof which is causing damp in the maternal unit
Medical Provision: There are an average of 330 outpatients a month and the main conditions seen are skin, respiratory tract and urinary tract infections, intestinal worms and asthma. The dispensary provides basic medical services including maternal health and under 5s clinics, a TB program and testing for HIV and malaria. There are 5 staff, including a clinical officer, two nurses and a laboratory assistant.
Medical equipment is very poor – this is a baby cot which is used once a baby is delivered
Inter Care’s impact: Inter Care has worked in partnership with Chekereni Dispensary since 1999, providing medicines and healthcare good which are given free to the many poverty stricken patients.
One of Inter Care’s founders, Patricia O’Keefe opened up this dispensary and there is a plaque placed on site in her honour
St Joseph’s Dispensary, Uchira
St Joseph’s is a small dispensary providing services for a poor catchment population of approximately 7000 people. The unit is only 11 kms outside of Moshi but is very remote and is accessed via a very bumpy, dirt track. The buildings are very run down and in need of repair. Medical equipment and medicines are in very short supply.
The roads were are full of rubble and is hard to navigate
Medical Provision: The dispensary provides basic medical services such as treatment of various infections, minor surgeries for trauma and rapid diagnostic testing for TB, HIV, malaria, pregnancy and urinalysis. There is one resident Clinical Officer and a few nurse assistants.
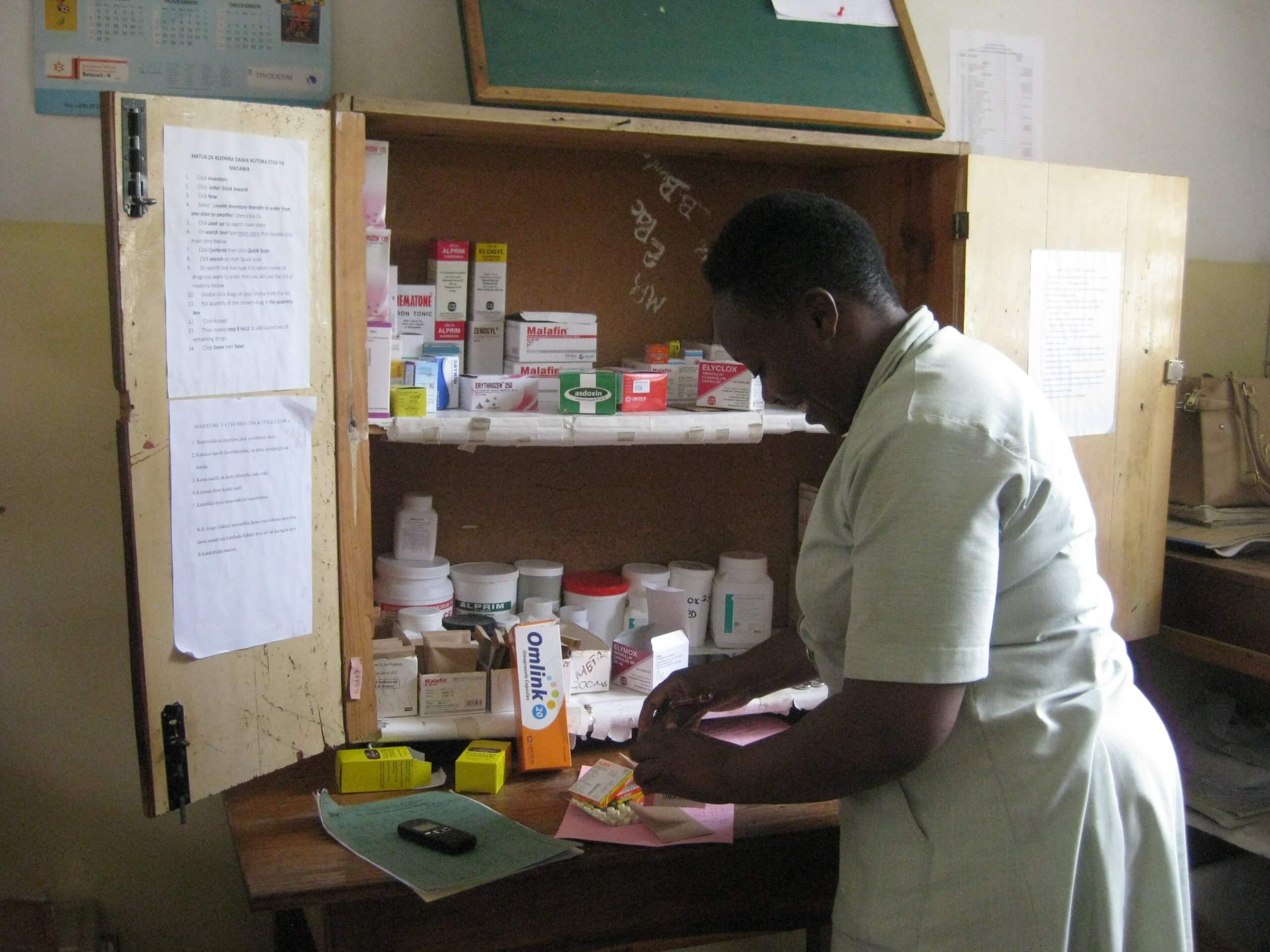
Nursing Assistant in the pharmacy
Inter Care’s impact: Inter Care has a long standing relationship with St Joseph’s Dispensary and have supplied medicines and healthcare goods for many years.
Huruma Hospital
Huruma Hospital is a large 250 bed Hospital which provides a wide range of medical services and procedures. It is 70 miles from Moshi and is situated near to the border with Kenya. The catchment population is about 300,000 and they treat patients from Tanzania and Kenya.
Medical Provision: The Hospital is comparatively well equipped and has some modern buildings such as the HDU (high dependency unit) but they do not have sufficient staff to deliver their services. Some of the staff are inadequately trained. Huruma struggles with an inconsistent water supply which makes providing services very challenging. They see lots of road traffic accidents, but do not have a CT scanner and have to refer patients to a regional hospital in Moshi.
Due to low water supplies, medical items are difficult to clean
Inter Care’s impact : Inter Care has worked in partnership with Huruma Hospital since 2006, providing medicines and healthcare good which are given free to the many poverty stricken patients.
We met Veronica who benefited from a post-natal care package donated by Inter Care (Visit in 2022). She comes from a low income family.
Kilema Council Designated Hospital
This hospital is in a very rural setting, in the foothills of Mount Kilimanjaro and 52 kms from Moshi in Northern Tanzania. There is severe poverty and high unemployment in the catchment area.
They face many challenges due to high unemployment in the area and the fact that many patients are unable to pay for the treatment they receive. The hospital faces a daily shortage of medicines and healthcare goods. The rural setting also contributes to the difficulties as the catchment population is approximately 217,000 people and the nearest Regional Hospital is KCMC (Kilimanjaro Christian Medical Centre) in Moshi.
The view from outside of the hospital
 Many people in this area are farmers. Banana trees are plentiful.
Many people in this area are farmers. Banana trees are plentiful.
Medical Provision: Kilema is a large facility with 12 doctors and 149 staff in total. It has 150 inpatient beds and a very busy outpatient department with an average of 1700 outpatients a month. As well as running routine clinics for such things as maternal health and TB, it also runs specialist clinics for dentistry, diabetes and hypertension. There is a basic ophthalmology department which is very under resourced.
The Eye Department has poor resources
Inter Care’s Impact: Inter Care has supported Kilema Hospital for many years with healthcare goods and medicines. In March 2023 we shipped a slit lamp, lens meter and trial lenses for use in their Ophthalmic Department. These significant pieces of equipment were donated to Inter Care.
Dr Godfrey Maro with donated Pulse Oximeters (Inter Care visit 2022)
St Joseph’s Hospital, Soweto
St Joseph’s is a very large, 17 doctor, 150 bed hospital with extensive buildings and many departments, including maternal/child health, dental and dialysis. It is situated in the centre of Moshi and it’s catchment area has relatively high levels of employment compared with other areas in Northern Tanzania. But, they face serious financial constraints – they struggle to purchase sufficient medicines and often buy on credit, and they lack the funds needed to train staff. Retention of staff is also a major problem as higher paid jobs can be found in Government run hospitals.
Medical Provision: St Joseph’s has a heavy workload with averages of 200 deliveries per month, 40-60 operations per month and 350 outpatients per week. The main conditions treated are pregnancy conditions, diabetes, hypertension, pneumonia and urinary tract infections.
Outpatients at the hospital
Inter Care’s Impact: Inter Care has supported St Joseph’s with healthcare goods and medicines since 2004. We have also provided some desperately needed items of equipment under the One Wish Project including Centrifuge Omega 12 tubes and a large number of stethoscopes.
Inter Care’s visit to St Joseph’s hospital (2022) and donated Pulse Oximeters to Sr Maria
St Mary’s Dispensary KIA
This Dispensary serves a very poor, rural community mainly made up of Maasai people. It is situated near to the airport in the Moshi region of Northern Tanzania. The health unit is lacking basic medical equipment and regularly runs short of vital medication.
Medical Provision: The dispensary runs many busy clinics including under 5s and maternal health, vaccinations and a TB program – there are 650 outpatients on average a month. The conditions most treated by the unit are urinary tract, gastrointestinal and respiratory infections and intestinal worms, but they also regularly see patients with other conditions such as hypertension and diabetes. The dispensary supports a large number of women through delivery and maternal health services.
Labour Ward
Medical Staff: St Mary’s is managed by Veronica Mboya, the Nurse Officer in charge, who has been there 22 years and lives on site. The government provides a Clinical Officer, but the main clinician is Dr Fulgence Makuta, who works at the dispensary as a volunteer three times a week. A dental technician from Kibosho Hospital visits once a week.
Sr Veronica with a microscope donated by Inter Care
Inter Care’s Impact: Inter Care has supported St Mary’s Dispensary with healthcare goods and medicines since 2006.
Inter Care’s visit to St Mary’s Dispensary KIA (2022) and meet the Maasai Tribe
St Francis of Assisi School and Dispensary
The school is in a rural setting just 4.5kms outside of Moshi. It is a boarding school for able bodied children and for children with Albinism and other disabilities. There is a large stone wall surrounding the school and high security on the entrance gate – in order to keep the children safe and specifically, to prevent the abduction and murder of children with Albinism. There is a dispensary within the school, which serves the children and the local poverty stricken community. The school provides a safe and caring place for the children but there are many serious issues, including a shortage of food and a lack of medicines and medical equipment.
The children welcome Inter Care on their visit in 2022 and sing for them
Medical Provision: The dispensary runs audiology and eye clinics and provides first line medical care for the school and community. There is a small medical team, including a visiting doctor, a full-time clinical officer, a nurse and a laboratory assistant.
The main conditions which they treat are pneumonia, diarrhoea, urinary tract, upper respiratory tract and other infections. In addition, they see hypertension and diabetes in adults. Serious cases are sent to their nearest referral hospital, which is 8 kms away and this often means a very uncomfortable transfer for the patient by rickshaw. They also provide anti natal and maternity services.
Children get their hearing tested
Inter Care’s Impact: Inter Care has supported St Francis’ School and Dispensary since 2004, providing healthcare goods and medicines.
Kilema Hospital
Report – Visit in 2011 (volunteer trip)
Nearly the whole party visited Kilema with a view to walking in the hills after the visit. Those of us who had visited Kibosho were impressed by the condition of the road for the first few km after leaving the tarmac of the Arusha Road, this however soon changed as the condition became increasingly rough. It is a journey worth making even if not to visit the hospital as the views from there are magnificent.
What we did first
We were greeted by Sister Clarissa, who was, unfortunately, unaware of our visit. She handed us over to another sister who took us on a tour of the hospital. It became increasingly apparent that a group of 16 is far too many to take round a hospital and most of the volunteers who were not immediately involved enjoyed the sun in the hospital garden for some of the visit.
At first glance
The hospital is well laid out and appears to be well run. They have male, female, obstetric and gaenological wards in addition to maternity and children’s wards and an out patient department. They see around 70 patients per day. There is also perform major surgery and have visits from an eye surgeon. The theatre is well laid out and reasonably well equipped; they do however need more sterile gloves and suture materials. On our trip round the hospital we were shocked to see that although we send up to date MIMS and BNF they were still using copies from 2003.
There also a lot of cases of intestinal worms and they asked us to send out albendazole. Inter Care does not routinely receive this and we would have to buy it.
The government supplies them with ARVs yet they do receive enough for their patients. At the moment they have 1,800 HIV positive patients and whilst the number is increasing it is now slowing down mainly due to extensive educational programmes. The government does not supply drugs for opportunistic infections and if able, patients pay for these.
They have an orphan support scheme which gives help to 210 orphans providing them with food and education (the word orphan often means a child who has lost one parent) many are orphans as a result of AIDS and are being cared for by grandparents or older siblings. The program encourages the children to remain within the community with family members and does home visits.
Final comments
We were then taken to the canteen and provided with lunch.
On saying goodbye to the hospital staff we were then taken to Marengu Falls which is a tourist attraction of the area.
Kibosho Hospital
Kibosho Hospital is in a very rural setting in the foothills of Mount Kilimanjaro in Northern Tanzania. Moshi is only 16kms away, but the journey is slow and particularly rough for the last 2 kms of road, which is a bumpy dirt track. There is no public transport to the hospital and many patients travel there on foot or by motorbike.
Nearby village – people travelling to the hospital via motorbike
Medical Provision: The hospital is a large, 180 bed facility with 11 doctors, 41 nurses and a total of 72 staff. It is managed by the Doctor in Charge, Dr John Materu. There is a particularly impressive ophthalmology department which is very busy and comparatively well equipped. Kibosho Hospital provides a full range of services, including child and reproductive health and programs for TB, Leprosy and HIV. They also give mental health and oncology provision. However, the hospital faces serious financial constraints and they struggle to fund services and medical supplies.
Franka is one of the many patients who cannot afford to pay for their treatment. Kibosho Hospital struggle to provide care for these people without Inter Care’s support.
Inter Care’s Impact: Inter Care has worked in partnership with Kibosho Hospital for many years, providing medicines and healthcare good which are given free to poverty stricken patients. In March 2023 we shipped a 3D Optical Topmography Machine to Kibosho for use in their Ophthalmic Department. This significant piece of equipment was donated to Inter Care.
St Camilius Health Centre, Mvimwa
This health centre is situated in Zanzibar. The main religion on the Island of Zanzibar is different from mainland Tanzania in that the population is 99% Muslim. There are 2 Catholic Dispensaries; one of which is supported by Inter Care, the other we were going to visit with a view to start supporting the unit.
Unlike the health units in the Mara region close to the Kenyan border the issues here are different. The Diocese of Zanzibar is small. It had little income for medicines.
In summary, our support ensures that they are able to invest in their facilities. This is an excellent example of the way in which our aid is not merely alleviating acute need, but helping our partners to help themselves.
(visit 2017)
Kwediboma Health Centre
Location: 120km East from Korogwe
Catchment population: 9-10,000
Key staff met: Sr Matilda
Nearest referral unit: 60km at Handeni
Facilities: 26 Beds, 5 wards (1 Masai if needed). No Transport. Have Lab, maternal/child health clinic, Mobile outreach clinic (once per week to administer vaccines and antenatal) and TB and HIV/AIDs program.
Staff: 3 Clinical Officers, 1 Pharmacy Assistant, 2 Nurses which are also Midwives, 18 Nursing Assistants.
Workload: 70-80 deliveries/ month + 70+ outpatient/day and 200+ inpatients per month.
Disease pattern: Malaria, URTI, Typhoid, Pneumonia, UTI, Anemia, Hypertension, Diabetes.
Support from government and other sources: Government supply Vaccines, HIV & TB medication, they also provide wages. Receive some UK Church based financial support.
Baraki Health Centre
Overview
Based on a complex including a big working farm and a school; 60 kms from Musoma and supports a population of 29,860. It felt like we were in the middle of nowhere. The countryside surrounding the health centre was extremely barren and there had been drought here for 2.5 years. Like the other units in this area, tribal customs and culture are a huge issue for them as patients often arrive too late for treatment. Patients often cannot afford to pay and the government supply no assistance so they are struggling with resources such as medicines and equipment. Inter Care’s impact was very evident to see here how we do assist in their work.
Grounds at Baraki Health Centre
Communications have been a major problem when liaising with Inter Care in the past. We now have the correct information but need to take note of their request for us to communicate with WhatsApp. The level of English spoken here was excellent, as many of the Srs from the convent had lived in England. There was a Dutchman volunteering on the farm whilst we visited.
Bikira Maria Mama Wa Tumaini Health Centre, Masanga
Overview
When Inter Care first visited to check this unit’s suitability for support in September 2017 we found it a large health centre with 65 beds across 5 wards. Located in a very remote region next to the Kenyan border and on the edge of the Serengeti National Park, the unit is surprisingly difficult to access due to very poor quality roads.
This centre has 24 fully qualified staff. These include 2 resident doctors, 5 clinical officers, a pharmacist and pharmacy assistant, 4 nurses and 6 midwives. Even though there is plenty of staff, they still meet various challenges. This is because the centre serves a catchment population of in excess of 16,000 treating 6,250 adults per year, 5000 teenagers and 1100 under 12 years. They see 100 plus Outpatients and look after almost 300 Inpatients each month.
Staff
Sr Bibiane Nzali, Director / Administrator in charge of running the centre is from the Congo. We found her to be extremely driven towards delivering their health projects. Furthermore, she was proud of winning funding resulting in the construction of a new theatre block. It was almost complete at the time of our visit. And this upgrade will enable the Health Centre to apply for Hospital status.
Conclusion
As we toured the centre, Sr Bibiane told us about the cultural issues with witch doctors and local customs. They raise problems for patients receiving treatment in this region. In addition to this, malnutrition is a serious problem. The health centre is able to provide porridge to their overnight patients.
In some months they have difficulties being able to afford to buy enough medical supplies and medicines. We concluded post visit that the health centre comfortably met Inter Care’s criteria. We now regularly support with basic medicines and dressings, in line with their specific requests. Sr Bibiane commented that “they appreciate the help from Inter Care”, adding, “ local people are really poor and need to be helped”.
Rainbow Centre, Moshi
The Rainbow Centre is housed in an old chapel in the centre of Moshi and is surrounded by the bustling city. It provides free HIV testing, counselling and support by way of a drop-in centre which is open Monday – Friday, 8.30am – 3.30 pm.
The building used to be a chapel
Medical provision and other services: Dr Materu (from Kibosho hospital) visits the centre when needed to provide medical care for AIDs patients who have other opportunistic conditions and infections. Patients also bring prescriptions to the centre and receive free medication.
The Centre is run by Sr Winfrida Alfajiri, the programme co-ordinator and two other nurses/counsellors. The program provides free AIDs testing facilities and counselling/education services but also gives community support by way of home bed care services and support with food and medication. Orphans who are cared for in the community by family members (mainly grandparents) are given help with food, school fees, books and materials. The Centre seeks to encourage people to become self-sufficient by giving grants to establish small income generating projects, such as growing crops, poultry keeping and small-scale farming.
They have volunteers working in the community who dedicate their time and skills for free. There are 76 volunteers (many of whom look after patients who are taking ARVTs), 18 peer educators and 5 co-ordinators. The Rainbow Centre covers a catchment area of 1,539,321 people, spread over 5 zones in the Moshi area. They have 1680 outpatients on average a month.
 The volunteers at Rainbow Centre have supported the local community with food and school books
The volunteers at Rainbow Centre have supported the local community with food and school books
Inter Care’s Impact: Inter Care has worked in partnership with The Rainbow Centre for many years, supplying desperately need medicines and healthcare goods.
Sr Winfrida shows us their low supply of medicines (Inter Care visit 2022)
Kibara Hospital
Kibara is a small rural hospital in a poor and deprived area. It is situated on a peninsula jutting out into Lake Victoria and is accessed by a 4 hour drive from the nearest city, Mwanza.
The hospital has 102 beds spread over its five wards serviced by 51 staff including 2 resident doctors and 16 nurses. They treat in the region of 400 Outpatients and care for 200 Inpatients each month. We find the key challenges faced by this hospital are similar to those faced by so many other partner health units Inter Care support – funding and infrastructure.
Kibara seriously lacks adequate and regular funding and has ongoing problems with its electrical supply. This was very evident to us when shown around wards with no lighting – we couldn’t really see what we were being shown (!). Staff bluntly explained “this is due to the cost of workers’ salaries and the Government failing to finance as was previously promised”.
Their medical needs are predominantly for antibiotics, which are in short supply due to the prophylactic treatment of HIV/AIDs patients, and them not being effectively supplied by the Government. In this part of the world hospitals have to pay excessive prices for their healthcare goods e.g. a single bandage cost £13. We know from experience that catheters and surgical equipment are also very expensive to buy in Tanzania and they too are much needed by this Hospital.
Overseas visits like these confirm to Inter Care’s management that our targeted medical aid is directly meeting local needs. Kibara continues to receive bi-annual consignments of aid to supplement their needs.
Mr. Nyamima, Nursing Officer in Charge commented “The support you give to us is very helpful to the hospital and its patients. Please continue to help the community improve their health status. Thanks, God bless you all”
Mercy
 Mercy is a 16-year-old young woman, who lives 20 km from Kibara Hospital. During her recent pregnancy she attended her local dispensary initially for her antenatal care, but then had to be admitted to the hospital for the childbirth.
Mercy is a 16-year-old young woman, who lives 20 km from Kibara Hospital. During her recent pregnancy she attended her local dispensary initially for her antenatal care, but then had to be admitted to the hospital for the childbirth.
The good news is that she had a healthy baby boy weighing 3kgs who is doing very well. The bad news was that she was suffering from pre-eclampsia – a condition which pregnant women can develop and is marked by high blood pressure in women who haven’t had high blood pressure before. Although Mercy went to full term her blood pressure was so high: 200/120++ that even 4 days post-delivery her blood pressure was still raised, also she still displayed significant oedema particularly around her ankles.
During her antenatal care, she had never once had any screening test for proteinuria as there were no strips available. This test would have enabled a fast diagnosis and treatment for the pre-eclampsia hence, avoiding the risk of serious complications which can affect both mother and baby. Luckily the outcome for Mercy and her baby was positive but it could just as easily not been. A simple urine test was all that was needed. Inter Care would like to help in the future by offering urine testing strips to the partner health units such as Kibara, to help young pregnant women just like Mercy.
Kitope Dispensary
It was clear evidence of what a Dispensary of similar size and catchment population (around 11,000) without Inter Care support looked like, versus one that does have our support.
Their facilities were lacking and what little they did have was of a poor quality. The British National Formula (BNF) that was on the Clinical Officer’s desk (who is also the resident Father of the community) was dated 2007, some 10 years out of date.
The unit is a typical Dispensary that fits the Inter Care model where we are able to improve the lives of its patients by providing resources such as medicines, small equipment and health care goods.
(Visit, September 2017)
St Camillus Dispensary, Tomondo
This is situated on the Island of Zanzibar. There are 2 Catholic Dispensaries; one of which is supported by Inter Care. Unlike the health units in the Mara region close to the Kenyan border the issues here are different.
The Diocese of Zanzibar is small and has little income to spend on medicines, yet we were pleasantly surprised, by the facilities at St Camillus Dispensary. This could have something to do with it being a building that they moved into as their previous Dispensary underwent an attack on the priests and the Dispensary and Church on Christmas Day in 2013 and was burnt to the ground.
It was clear though that the monies that they had saved on not needing to purchase medicines and health care goods that had been donated by Inter Care, meant they could invest in their facilities.
This is an excellent example of the way in which our aid is not merely alleviating acute need, but helping our partners to help themselves.
(Visit, September 2017)
Bukwali Dispensary
Overview
Run by William Kahwezi this is a very remote dispensary off the North West part of Lake Victoria and next to the Ugandan border (4kms).
Inter Care started supporting the dispensary after an earthquake hit the region 2016. It suffered a lot of damage to the building and local infrastructure.
William the Clinical Officer In Charge, has been there for 46 years. He specialises in Ophthalmology and was the first medic to refer a patient to the Department of Health back in 1984. This patient turned out to be the first patient diagnosed with HIV in Tanzania.
William lives across the road. His wife used to deliver the babies and his two daughters also work there. It has a family run feel to it.
Case Study
Zola, a 36 year old woman lived nearby with her four children and during the middle of night their home set on fire. The children managed to escape, however, Zola got badly burnt.
HOWEVER William was able to treat her with the dressings and medication Inter Care supplied and he truly believes that they actually saved her life.
She is now living in a UN emergency shelter with her children. She is coping relatively well and the scarring is minimal. Also it was a miracle she didn’t suffer any secondary infections.
(Visit, September 2017)
Makongoro Health Centre (AICT), Mwanza
A very active Evangelical body of people known as AICT (African Inland Church of Tanzania) has established several medical units in Northern Tanzania. Inter Care has been sending supplies through to Makongoro Health Centre since 1992. They collect directly through Mwanza airport as they have a permit to clear customs and they distribute the consignment between the units as needs dictate but the majority goes to the health centre we visited in Mwanza.
They have a high standard of care and integrity which was clear to see with the personnel we met. They, like the majority of units visited are struggling with finances. They have built an operating theatre ready for abdominal surgical procedures, including deliveries and caesarean sections but have run out of money to equip and staff it.
The equipment they did have was in a poor state and in need of replacement. A Canadian nurse (from World Renew) has been working there for 6 years and clearly has a big impact within the health unit. There were not many medicines on the shelves and they have had problems with the quality of certain medicines therefore have a policy, for certain conditions such as diabetes, only to buy the medicines from Europe.
(Visit, September 2017)
Sayusayu Dispensary
We travelled 120kms from the Main gate of the Serengeti to reach this Dispensary. It literally is miles from anywhere. The last 58km from Old Maswa is on a dirt track and the last 4kms from Maswa Town was on very rough road, which is clearly impassable in the rainy season.
50% of the local population are HIV positive and malaria is a big problem in this inland region. The local Parish Priest, Fr Albert Izengo with the help of 2 Clinical Officers, runs this 27-bedded unit. Sisters from Rwanda who have difficulties speaking Swahili and spoke no English support them.
Case Study: This was lucky for Bina who is 5 years old and her mother who live some 40kms away. Sadly, the upper part of Bina’s body was badly burnt after she fell playing near a fire and after some time being treated at a hospital she is now in the care of the Dispensary. Her family could no longer afford treatment at the hospital so went to Sayusayu for her recovery and physiotherapy. She has very little movement in either arm but they are currently working on trying to stretch her right arm using a simple cloth to tie her arm to stretch the skin. The left arm appeared to be much worse. Bina is having some pain relief when needed. Her recovery will take months and her parents are very poor.
She is receiving treatment with the help of Inter Care donating pain relief and dressings to treat the burns.
(Visit, September 2017)
Nyarambo Health Centre
This 18-bed unit supports a very widespread population of 24,833 who are mostly subsistent farmers living off less than $1 per day. The health centre is located 1 hour north of Tarime on a rough road. Inter Care donations are clearly very valued here too as the day before we arrived Sr Josephine (In Charge) had badly broken her wrist and, admitted to the nearest hospital (one hour’s drive away in Shirati), discharged herself to ensure that she was in attendance herself to meet with us.
This was most definitely the poorest centre we visited, as its facilities were in very poor condition, there were no sheets on the beds and the mattresses were torn to shreds. Although September is the quietest month in the region for patient numbers – there were many patients around this centre receiving treatment.
(Visit, September 2017)